Blog
What a Podiatrist Treats

A podiatrist is a medical specialist who focuses on diagnosing and treating conditions of the feet and ankles. They manage a wide range of problems including bunions, fungal infections, ingrown toenails, and diabetes-related foot complications. Bunions appear as a bony bump at the base of the big toe, and may cause pain or misalignment. Fungal infections can lead to thick, discolored nails or skin irritation, and ingrown toenails occur when the nail grows into the surrounding skin, causing redness and discomfort. Diabetes-related foot complications encompass a range of conditions, including neuropathy, poor circulation, ulceration, infection, and impaired wound healing. A podiatrist can provide an accurate diagnosis, advanced treatment options, and ongoing care to improve foot health and prevent complications. If you have foot or ankle pain, it is strongly suggested that you visit a podiatrist for an evaluation and appropriate treatment options.
If you are experiencing pain in the feet or ankles, don’t join the stubborn majority refusing treatment. Feel free to contact one of our podiatrists from Florida. Our doctors can provide the care you need to keep you pain-free and on your feet.
What Is a Podiatrist?
Someone would seek the care of a podiatrist if they have suffered a foot injury or have common foot ailments such as heal spurs, bunions, arch problems, deformities, ingrown toenails, corns, foot and ankle problems, etc.
Podiatric Treatment
A podiatrist will treat the problematic areas of the feet, ankle or lower leg by prescribing the following:
- Physical therapy
- Drugs
- Orthotic inserts or soles
- Surgery on lower extremity fractures
A common podiatric procedure a podiatrist will use is a scanner or force plate which will allow the podiatrist to know the designs of orthotics. Patients are then told to follow a series of tasks to complete the treatment. The computer will scan the foot a see which areas show weight distribution and pressure points. The podiatrist will read the analysis and then determine which treatment plans are available.
If you have any questions, please feel free to contact our offices located in North Miami, and Pembroke Pines, FL . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Achilles Tendon Pain Can Affect Daily Movement
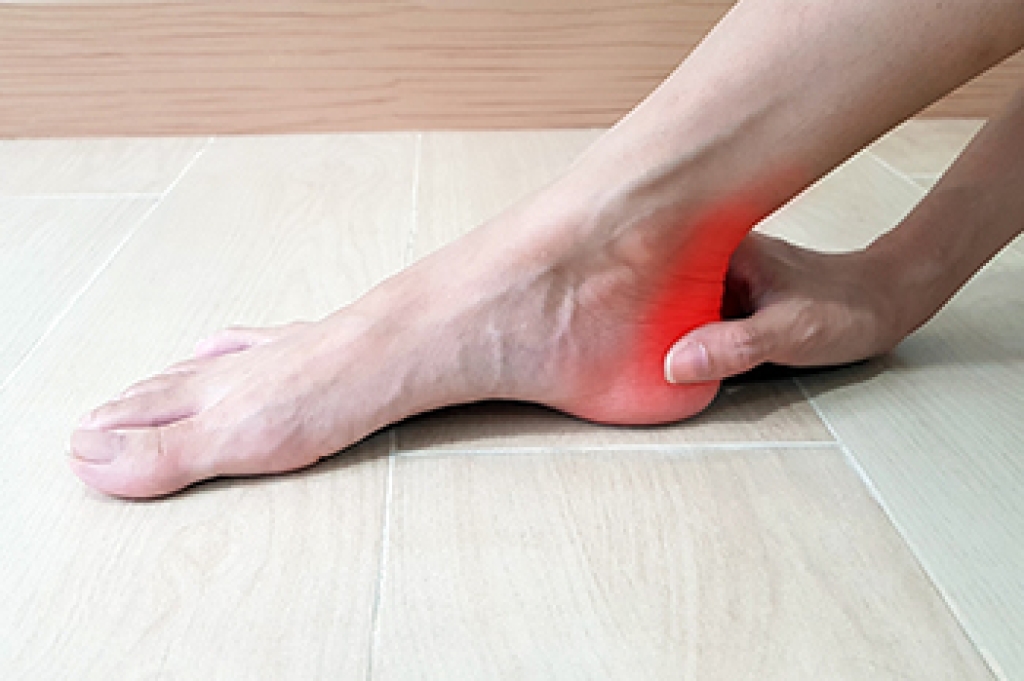
Achilles tendon pain often develops when the thick tendon connecting the calf muscles to the heel becomes irritated or inflamed from overuse, strain, or injury. This condition may cause aching, stiffness, or burning pain along the back of the heel or lower leg. This often happens after exercise or first getting out of bed in the morning. The area may appear swollen or thickened and can feel tender when touched. Running, climbing stairs, or prolonged walking may increase discomfort and make movement more difficult. Common causes include sudden increases in activity, tight calf muscles, wearing improper footwear, and repeated stress on the tendon. A podiatrist can evaluate the severity of the condition and determine whether there is inflammation, small tears, or tendon degeneration. Treatment may include wearing supportive footwear, targeted exercises, and activity modification. If you have Achilles tendon pain, it is suggested that you schedule an appointment with a podiatrist for an accurate diagnose and appropriate treatment plan.
Achilles tendon injuries need immediate attention to avoid future complications. If you have any concerns, contact one of our podiatrists of Florida. Our doctors can provide the care you need to keep you pain-free and on your feet.
What Is the Achilles Tendon?
The Achilles tendon is a tendon that connects the lower leg muscles and calf to the heel of the foot. It is the strongest tendon in the human body and is essential for making movement possible. Because this tendon is such an integral part of the body, any injuries to it can create immense difficulties and should immediately be presented to a doctor.
What Are the Symptoms of an Achilles Tendon Injury?
There are various types of injuries that can affect the Achilles tendon. The two most common injuries are Achilles tendinitis and ruptures of the tendon.
Achilles Tendinitis Symptoms
- Inflammation
- Dull to severe pain
- Increased blood flow to the tendon
- Thickening of the tendon
Rupture Symptoms
- Extreme pain and swelling in the foot
- Total immobility
Treatment and Prevention
Achilles tendon injuries are diagnosed by a thorough physical evaluation, which can include an MRI. Treatment involves rest, physical therapy, and in some cases, surgery. However, various preventative measures can be taken to avoid these injuries, such as:
- Thorough stretching of the tendon before and after exercise
- Strengthening exercises like calf raises, squats, leg curls, leg extensions, leg raises, lunges, and leg presses
If you have any questions please feel free to contact our offices located in North Miami, and Pembroke Pines, FL . We offer the newest diagnostic tools and technology to treat your foot and ankle needs.
Facts About Tarsal Tunnel Syndrome
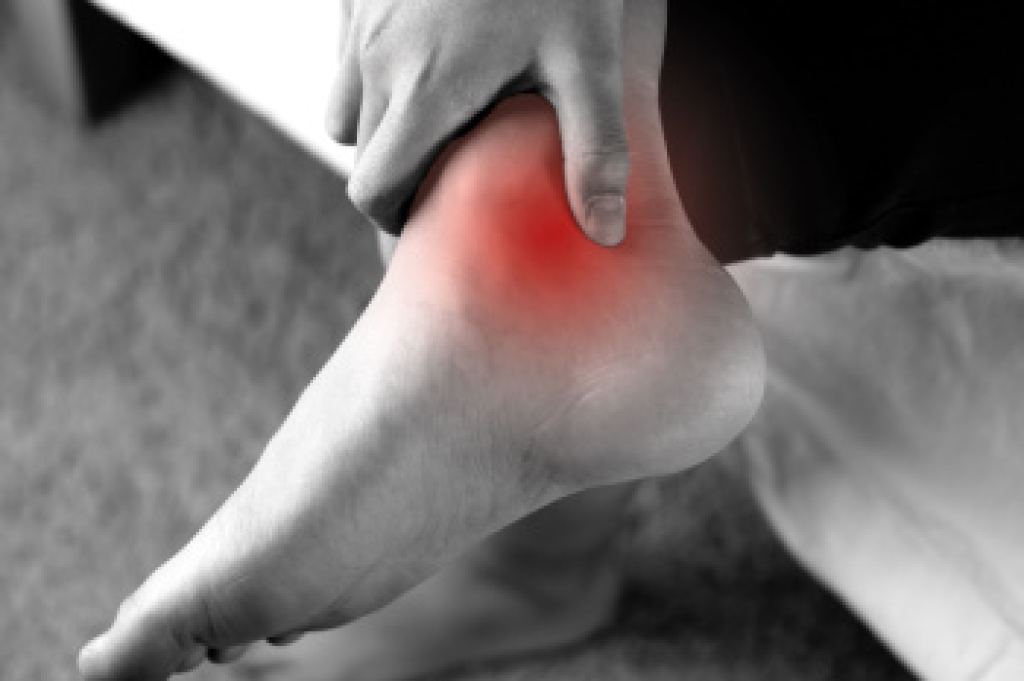
Tarsal tunnel syndrome is caused by compression of a nerve that runs along the inside of the ankle, leading to discomfort in the foot. Common causes include flat feet or fallen arches, swelling from an ankle sprain, and conditions like arthritis or diabetes that increase pressure in the area. Symptoms include tingling, burning, numbness, or shooting pain that can worsen with activity. Risk factors include poor foot structure, inflammation, and repetitive stress. Wearing compression socks may help reduce swelling and provide support, which can ease symptoms for some individuals. A podiatrist can evaluate the condition, recommend treatments, and address underlying causes. If you have any of the above symptoms, it is suggested that you consult a podiatrist who can offer effective relief and treatment solutions.
Tarsal tunnel syndrome can be very uncomfortable to live with. If you are experiencing tarsal tunnel syndrome, contact one of our podiatrists of Florida. Our doctors can provide the care you need to keep you pain-free and on your feet.
Tarsal Tunnel Syndrome
Tarsal tunnel syndrome, which can also be called tibial nerve dysfunction, is an uncommon condition of misfiring peripheral nerves in the foot. The tibial nerve is the peripheral nerve in the leg responsible for sensation and movement of the foot and calf muscles. In tarsal tunnel syndrome, the tibial nerve is damaged, causing problems with movement and feeling in the foot of the affected leg.
Common Cause of Tarsal Tunnel Syndrome
- Involves pressure or an injury, direct pressure on the tibial nerve for an extended period of time, sometimes caused by other body structures close by or near the knee.
- Diseases that damage nerves, including diabetes, may cause tarsal tunnel syndrome.
- At times, tarsal tunnel syndrome can appear without an obvious cause in some cases.
The Effects of Tarsal Tunnel Syndrome
- Different sensations, an afflicted person may experience pain, tingling, burning or other unusual sensations in the foot of the affected leg.
- The foot muscles, toes and ankle become weaker, and curling your toes or flexing your foot can become difficult.
- If condition worsens, infections and ulcers may develop on the foot that is experiencing the syndrome.
A physical exam of the leg can help identify the presence of tarsal tunnel syndrome. Medical tests, such as a nerve biopsy, are also used to diagnose the condition. Patients may receive physical therapy and prescriptive medication. In extreme cases, some may require surgery.
If you have any questions please contact our offices located in North Miami, and Pembroke Pines, FL . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
How to Recognize Toenail Fungus
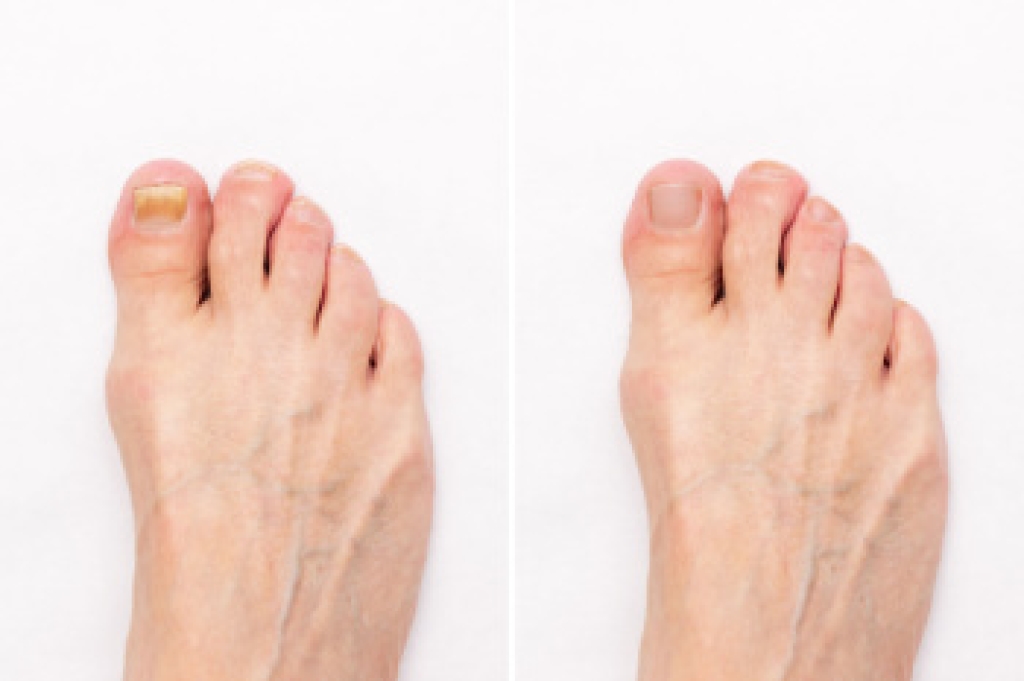
Toenail fungus often begins with small changes that are easy to miss. A common early sign includes a white, yellow, or brown spot near the tip of the toenail. The nail may also look dull, become thicker, or start to feel brittle and weak. As the infection spreads, the nail can separate from the skin underneath, which may cause discomfort when walking or wearing shoes. In some cases, debris can build up under the nail, and the nail may develop an unpleasant odor. Toenail fungus is more likely to develop in warm, moist places and can happen after nail injuries or from wearing tight shoes . A podiatrist can examine the nail, confirm if fungus is present, and provide treatment that includes trimming damaged nail tissue and prescribing antifungal medicine to stop the infection from spreading. If you have symptoms of toenail fungus, it is suggested that you schedule an appointment with a podiatrist for a diagnosis and appropriate treatment.
For more information about treatment, contact one of our podiatrists of Florida. Our doctors can provide the care you need to keep you pain-free and on your feet.
Toenail Fungus Treatment
Toenail fungus is a condition that affects many people and can be especially hard to get rid of. Fortunately, there are several methods to go about treating and avoiding it.
Antifungals & Deterrence
Oral antifungal medicine has been shown to be effective in many cases. It is important to consult with a podiatrist to determine the proper regiment for you, or potentially explore other options.
Applying foot powder on the feet and shoes helps keep the feet free of moisture and sweat.
Sandals or open toed shoes – Wearing these will allow air movement and help keep feet dry. They also expose your feet to light, which fungus cannot tolerate. Socks with moisture wicking material also help as well.
If you have any questions please contact our offices located in North Miami, and Pembroke Pines, FL . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.

